Skin, Inflammation, and the Cost of Ignoring Signals
Medical Disclaimer:
This post reflects my personal experience and interpretation of publicly available research. It is not medical advice, diagnosis, or treatment guidance. Hormonal health, neurological conditions, and inflammatory skin disorders are complex and highly individual. Always consult a licensed healthcare provider regarding medical concerns or treatment decisions.
For most of my life, my skin was clear. Not manageable. Not good-with-the-right-products. Clear.
Late 2023 was the first time that changed.
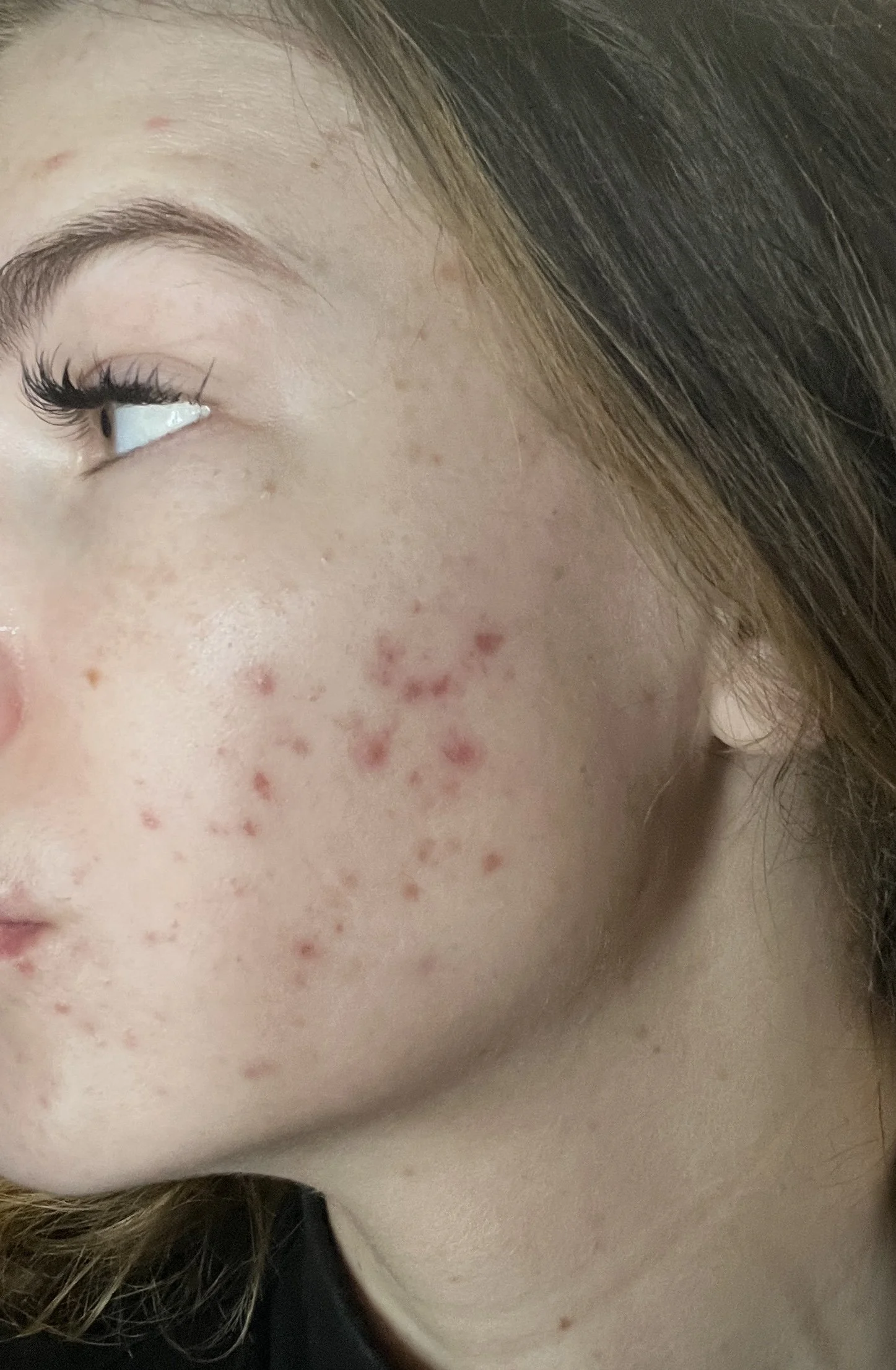
Breakouts began gradually and then escalated. By fall and winter of 2024, it was cystic and layered — multiple whiteheads forming within a single inflamed lesion, persistent redness, scarring. It felt less cosmetic and more systemic.
That distinction matters.
2022
The First Explanation
In early spring 2024, I stopped hormonal birth control. I had been on it for years — including several consecutive years of Depo-Provera injections. At the time, I assumed the acne was hormonal rebound or synthetic hormone disruption. That explanation felt logical, so I accepted it. In January 2025, I was prescribed a three-month course of tetracycline. I completed two months. There was no meaningful shift.
That should have told me something.
2024
2025
The Variable I Didn’t See
In late March 2025, what I thought was a sinus or ear infection escalated quickly. On April 1, I was admitted to The Ohio State University Wexner Medical Center ICU.
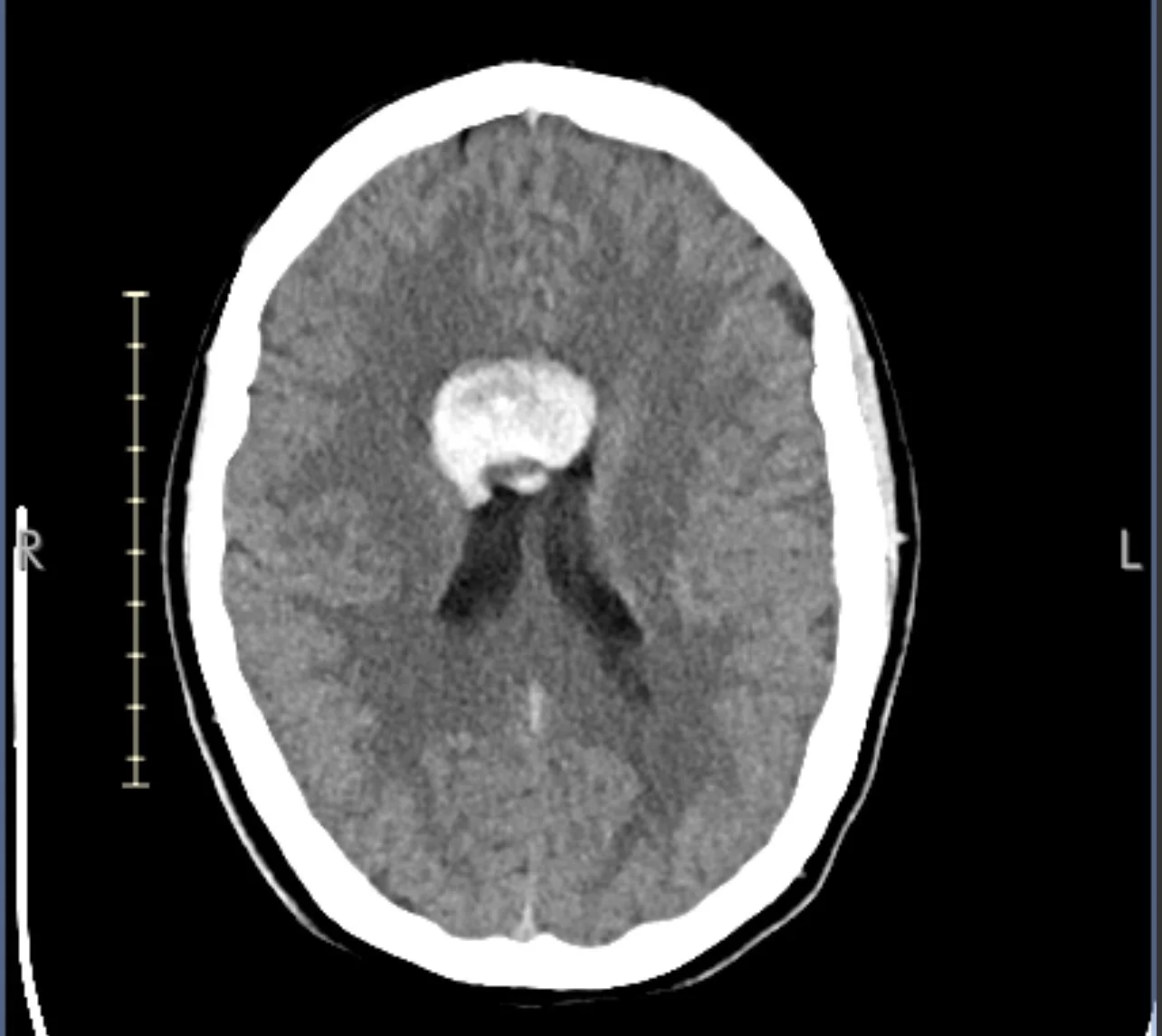
On April 10, surgeons removed a vascular malformation located in the ventricular space near the hypothalamus and pituitary region — the regulatory axis for hormones, stress response, and inflammatory signaling. I returned home April 12.
For twelve days in the hospital, I did not cleanse my face. No routine. No actives. No system. Within weeks of surgery, my skin began to clear. Quietly. Noticeably. The root problem had never been topical.
Vascular Malformation
April 12, 2025
The Estrogen–Oxygen Connection
In January 2026, I read two separate books by Ray Peat: Generative Energy and Nutrition for Women. The most striking concept in both was this:
He proposed that estrogen dominance creates a physiological state similar to oxygen deprivation — increasing inflammatory stress and metabolic inefficiency at the cellular level.
Whether one agrees with all of his frameworks is secondary. What stayed with me was the inflammation parallel. When I looked back at my timeline, the pattern became harder to ignore.
I had been on Depo-Provera for approximately three to five consecutive years earlier in my life. I was never advised at the time to cycle off or alternate methods. Years later, another physician told me extended continuous use is often monitored more carefully.
After I publicly shared about my brain mass, multiple nurses messaged me privately asking the same question:
“Had you taken Depo?”
That doesn’t prove causation. But patterns deserve to be examined.
Depo-Provera is a synthetic progestin (medroxyprogesterone acetate). It is not bioidentical progesterone — and Ray Peat’s work distinguishes heavily between protective progesterone and synthetic derivatives.
I don’t know which hormonal pathway dominated in my case. I do know that something in my endocrine environment was not stable.
And inflammatory skin was one of the earliest visible signals.
What Changed the Surface
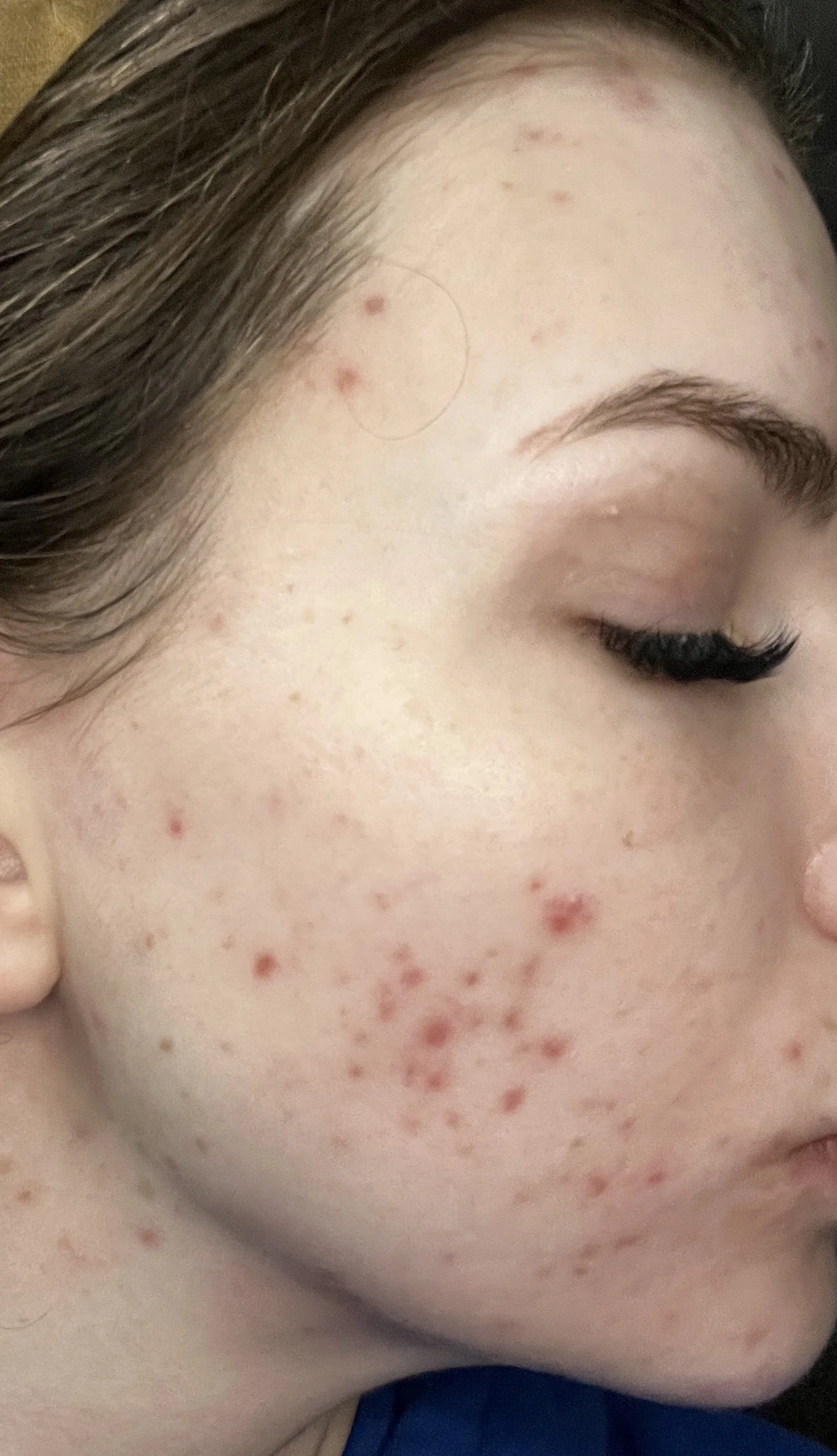
By late 2025, the acne was no longer explosive but still cyclical — appearing during high stress seasons or before my menstrual cycle.
In late December 2025, after listening to Dr. Barbara Sturm speak about chronic inflammation and skin on the The Emma Grede Podcast, I simplified my routine. Not optimized. Simplified.
I switched to:
Dr. Barbara Sturm Cleanser
Enzyme Cleanser (once weekly)
Hyaluronic Serum
Face Cream
No rotating acids. No layered actives. No aggressive corrections.
Within one month — January 2026 — the improvement was significant. Breakouts still occur under high stress or before my cycle. But they are smaller, less inflamed, and resolve faster.
Around the same time, I made two small systemic changes:
Vitamin E supplementation
Eating breakfast (two eggs and toast) before coffee to stabilize cortisol and thyroid signaling
Nothing aesthetic. Just lowering inflammatory load.
Dr. Barbara Sturm Routine
January 2026
The Larger Lesson
Acne is often framed as a surface-level disorder requiring surface-level escalation.
In my case, it was a signaling issue.
Hormonal instability. Neurological stress. Inflammatory load. Overcorrection.
The instinct when skin destabilizes is to intensify. The better move — at least for me — was restraint.
Simplify the surface. Reduce systemic stress. Watch for patterns.
Inflammatory skin does not benefit from aggression. It benefits from calm inputs.
I’m linking the exact Dr. Barbara Sturm products I currently use below. Clear skin, for me, was never about finding the strongest product. It was about reducing noise and paying attention to signal.
Clear skin, for me, was never about finding the strongest product. It was about reducing noise and paying attention to signal.
There is still work to be done. But the shift in just one month of lowering inflammatory load — internally and topically — has been significant. That alone tells me I’m finally moving in the right direction.